Breastfeeding After Birth
Learning Objectives
Knowledge and Understanding
- Breastfeeding after birth
- Counseling and supporting the mother and baby for first breastfeeding
- Breastfeeding after cesarean section
- Helping mothers breastfeed in prone position and side-lateral position
- Breastfeeding positions and signs of good attachment
- Spoon feeding
- Learning how to give paladai / suthi spoon feed to the baby
- Feeding cues of a normal baby
- Identify when a baby is ready to feed
- Identifying a sick baby
- Be able to identify when a baby is sick and requires doctor's care
Facilitators: Pediatrician, Lactation counselor
Group discussions with participants to understand their knowledge and attitude, followed by case scenarios and role plays.
Lactation counselors will organize hands-on sessions in small groups of trainees who shall counsel and provide breastfeeding support.
Training resources: Hospital setting of maternity ward having healthy newborns and mothers
Breastfeeding After Birth
Start breastfeeding counseling in antenatal period. Educate mother and family about the importance of good diet and nutrition of the mother for the health of the baby.
Evaluate mother's general health, breasts, and nipples. Treatment of flat or inverted nipples should be started antenatally so that breastfeeding can be started immediately after birth.
Mothers should be encouraged and supported to start breastfeeding within one hour of birth.
Immediate Post-Delivery Breastfeeding
Skin-to-Skin Contact
- Place baby directly on mother's abdomen after birth
- Dry the baby with a warm sterile sheet, except baby's hands
- Baby will soon find mother's breasts - Breast Crawl - and start breastfeeding
- Avoid mother-baby separation unless medical emergency
- Continue for at least one uninterrupted hour
Benefits of Early Initiation and Skin-to-Skin Contact
For Infant:
- Optimal temperature maintenance
- Colonization with maternal flora
- Enhanced immune protection
- Improved cardiorespiratory stability (delayed cord clamping)
For Mother:
- Enhanced bonding and attachment
- Improved milk production
- Reduced postpartum bleeding
- Lower risk of postpartum depression
- Increased confidence
What We Should Do?
Support, Don't Interfere:
- Minimize handling and procedures
- Keep mother and baby together
- Provide encouragement and reassurance
- Document feeding attempts and success
Assessment Without Separation:
- APGAR scoring can be done on mother's chest
- Initial examination while maintaining skin-to-skin contact
- Weight and measurements can be delayed
- Vitamin K injection after first breastfeeding
Hospital Practices for Success
Baby-Friendly Hospital Initiative Steps
- Written breastfeeding policy communicated to staff
- Training for healthcare staff in breastfeeding support
- Inform pregnant women about benefits and management
- Immediate skin-to-skin contact after birth
- Help mothers initiate breastfeeding within one hour
- Give infants only breast milk unless medically indicated
- Rooming-in 24 hours per day
- Encourage breastfeeding on demand
- No pacifiers or artificial nipples for breastfeeding infants
- Establish breastfeeding support groups and referral systems
Breastfeeding Positions
After Cesarean Section
Prone Position
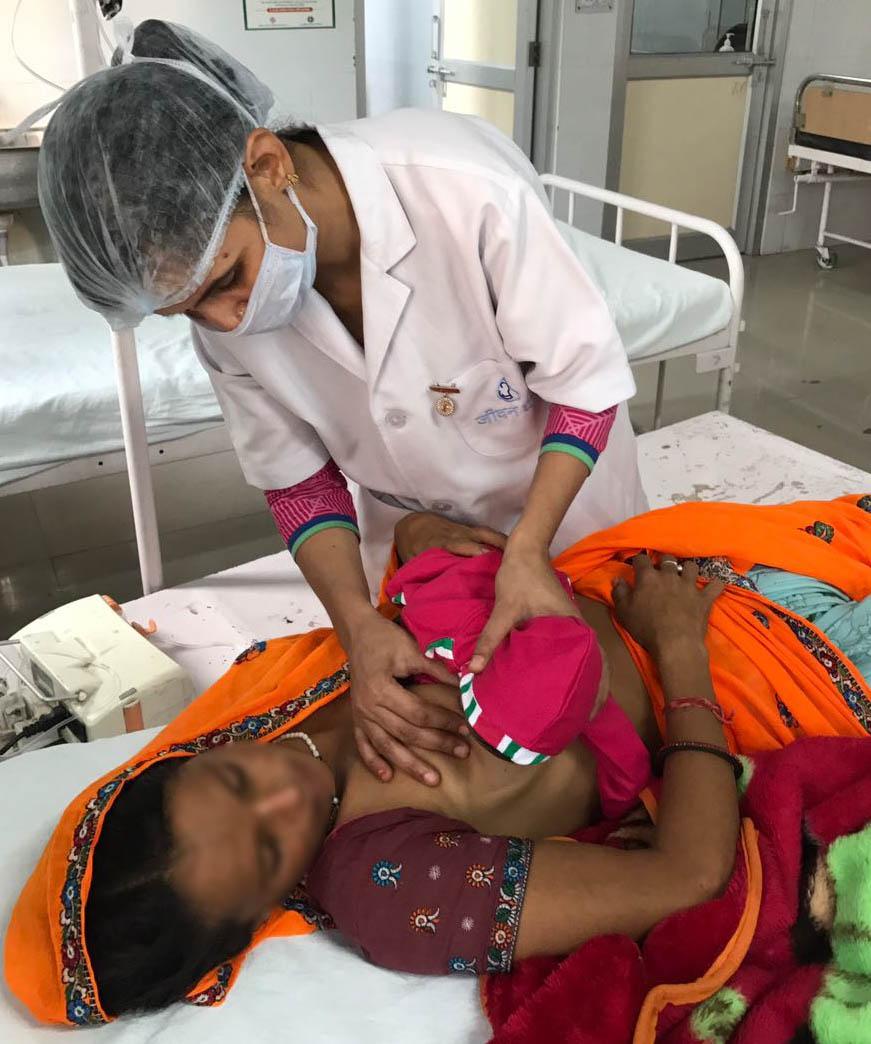
Mother needs a little support and encouragement to breastfeed after cesarean section. Support the baby in a prone position over the breasts and the baby will do the rest.
Prone Position Benefits:
- The baby is comfortable feeding in this position
- If the mother finds it difficult to support the baby in this position, counselors should initially support the baby
- Later, the family members can be encouraged to support the baby in a prone position
Lateral Position (From Second or Third Day)
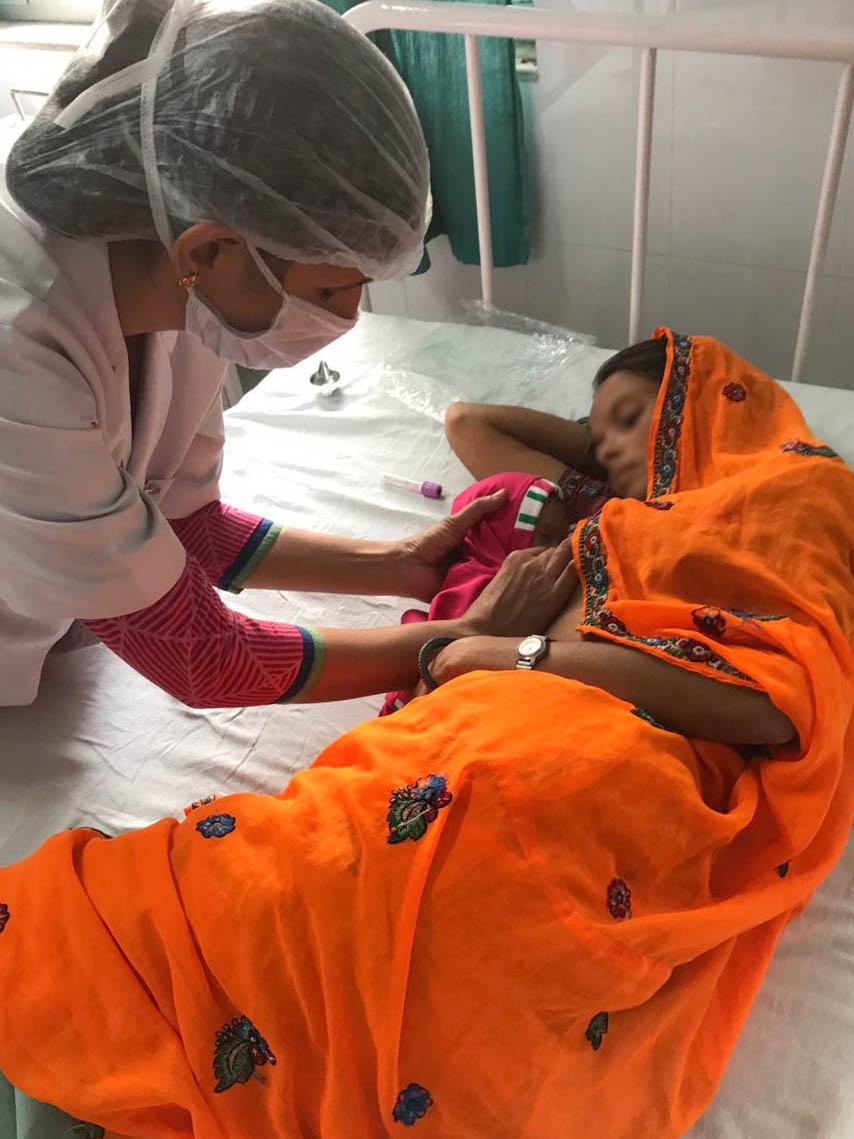
From second or third day, when the mother is comfortable, she can breastfeed in lateral position.
The baby still needs to be supported for proper latching
Other Positions
Good Positioning Characteristics
Mother:
- Comfortable and well-supported
- Back straight, shoulders relaxed
- Arms supported with pillows
- Feet flat on floor or footstool
Infant (सीधा सहारा सामने समीप):
- Body aligned (ear, shoulder, hip in line)
- Facing mother with whole body turned toward breast
- Close to mother's body
- Head slightly extended, not flexed
Positioning Techniques
Cradle Hold
Description:
- Most common and traditional position
- Good for experienced mothers and older infants
- Allows one-handed feeding once established
Technique:
- Hold infant with arm on same side as feeding breast
- Support infant's head in crook of elbow
- Infant's body lies across mother's lap
- Use opposite hand to support breast if needed
- Bring infant to breast when mouth opens wide
Best For:
- Term infants with good muscle tone
- Mothers comfortable with breastfeeding
- When privacy and discretion are priorities
Cross-Cradle Hold
Description:
- Good for learning proper latch
- Provides better head and neck control
- Recommended for newborns and small infants
Technique:
- Hold infant with arm opposite to feeding breast
- Support infant's head with palm of hand
- Thumb and fingers behind infant's ears
- Infant's body supported by forearm
- Use same-side hand to shape breast
- Guide infant to breast when ready
Best For:
- Newborns and premature infants
- Mothers learning to breastfeed
- Infants with latch difficulties
Football/Clutch Hold
Advantages:
- Good visualization of latch
- Keeps infant away from mother's abdomen
- Good for large-breasted mothers
- Allows feeding of twins simultaneously
Technique:
- Position infant at side, under mother's arm
- Support infant's head with palm
- Infant's feet point toward mother's back
- Use pillows to support infant's body
- Guide to breast with gentle pressure
Best For:
- After cesarean section
- Large or engorged breasts
- Small or premature infants
- Twins or multiple infants
Signs of Good Attachment

Proper latching is the key to successful breastfeeding. Getting a good breastfeeding latch can take some practice and support, especially for first-time mothers.
Observe the mother breastfeeding her baby and identify whether the baby is comfortable or not by checking these four signs of good attachment:
Four Signs of Good Attachment
-
Baby's mouth is opened wide
-
Lower lip of the baby is turned outwards
-
Chin of the baby is touching the breasts
-
More of the areola is visible above the baby's mouth than below it
Alternative Feeding Methods
Paladai Feeding
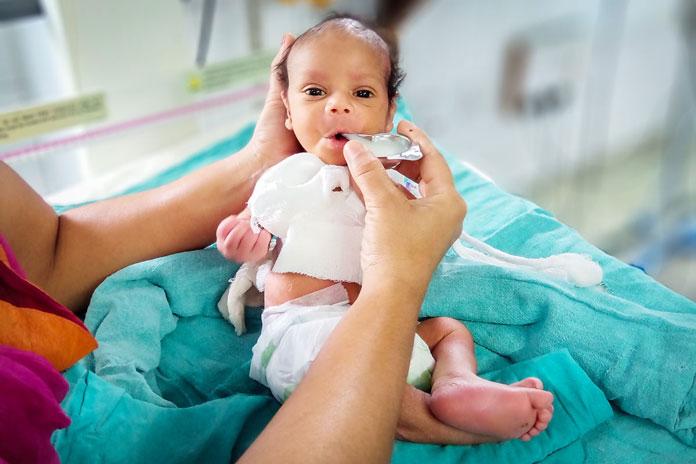
When direct breastfeeding is not possible, a mother can express her breast milk and feed the baby with a spoon or cup. A special spoon is available for feeding newborn babies, called suthi spoon or paladai.
When to Give Spoon Feeding
Maternal Health Issues:
- When the mother is unhealthy and unable to breastfeed directly
- If the mother has active tuberculosis or chickenpox infection, she can express her breast milk and feed by paladai
Premature Babies:
- Babies born before due date may not develop the sucking-swallowing coordination needed for direct breastfeeding
- Baby's doctor may advise giving paladai feeds in such cases
NICU Admission:
- When the baby is admitted in NICU
- Such babies may not be able to breastfeed due to their illness, but paladai feeding may be allowed by the doctor in some cases
Working Mothers:
- A working mother can express and store her breast milk
- Caregivers can feed this expressed breast milk with a spoon
How to Feed Using Paladai
Step-by-Step Technique:
- Support the baby in the lap in an upright position - keep the baby's neck slightly extended
- Take out some milk in sterile katori
- Fill suthi spoon (paladai) with milk
- Gently insert the tip of suthi spoon in baby's mouth and allow the baby to suckle the milk
- Do NOT pour milk into baby's mouth
Cup Feeding

Cup feeding is another safe alternative feeding method that does not interfere with breastfeeding technique.
Technique:
- Use small silicon cup with smooth rim and fill with milk
- Hold infant upright in your lap
- Touch rim of cup to infant's lips
- Tilt cup slightly so milk just touches the lips
- Allow the infant to lap the milk with tongue - do NOT pour
- Infant sets the pace of feeding
Advantages of Paladai / Cup Feeding
- Does not interfere with breastfeeding technique (unlike bottle feeding which causes nipple confusion)
- Suitable for premature babies (with doctor's advise)
- Easy to clean and sterilize
Feeding Cues of a Normal Baby
How will a mother know if her baby is hungry?
Babies have a unique language by which they communicate with their mothers. This language is basic and simple to interpret. When a baby demands feed, it is called as feeding cue.
Early Cues
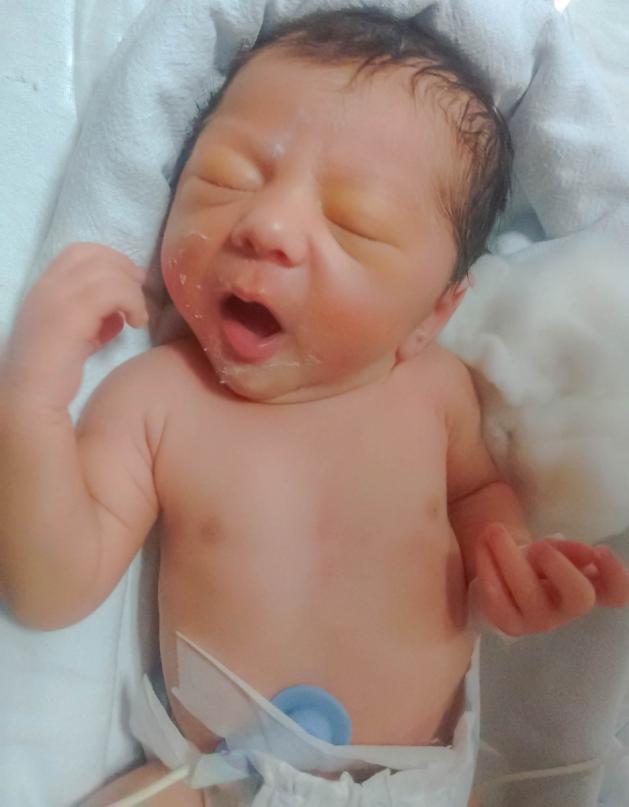
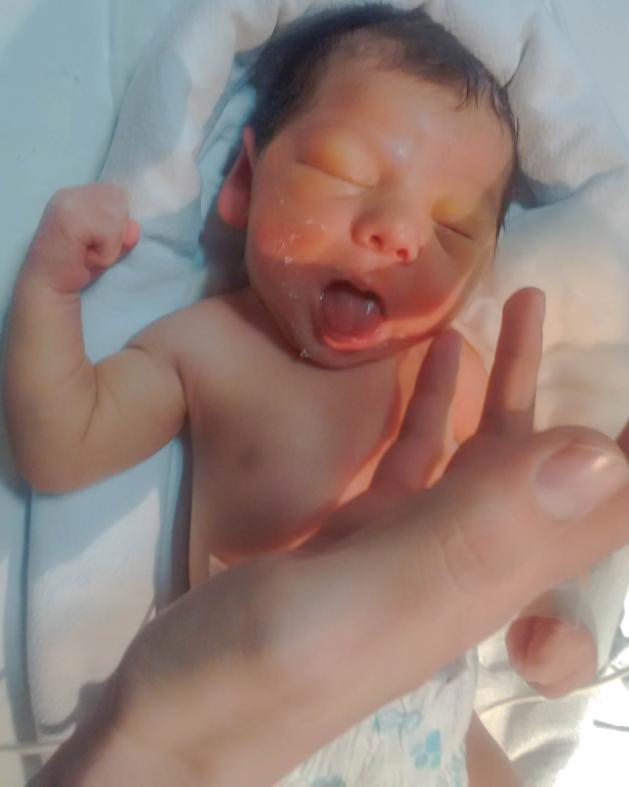
- The baby starts moving a little bit and intermittently opens their mouth
- The baby takes their tongue out and makes sucking actions
Action:
- Baby will comfortably accept feed at this stage and it is a good time to start breastfeeding
Additional Early Signs:
- Increased alertness: Eyes open, looking around
- Hand-to-mouth activity: Bringing hands to face and mouth
- Physical movement: Stretching, squirming
- Sound making: Soft cooing or murmuring sounds
Mid Cues
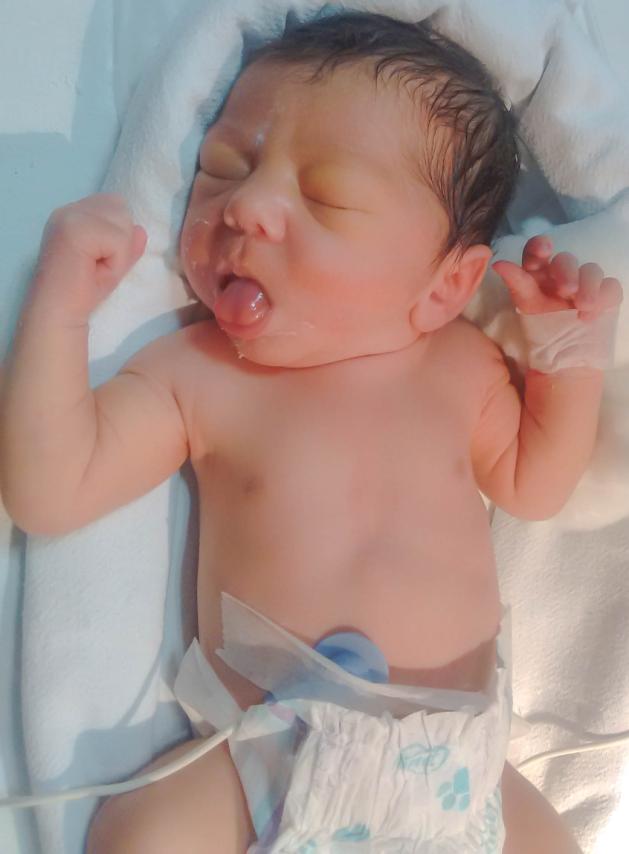
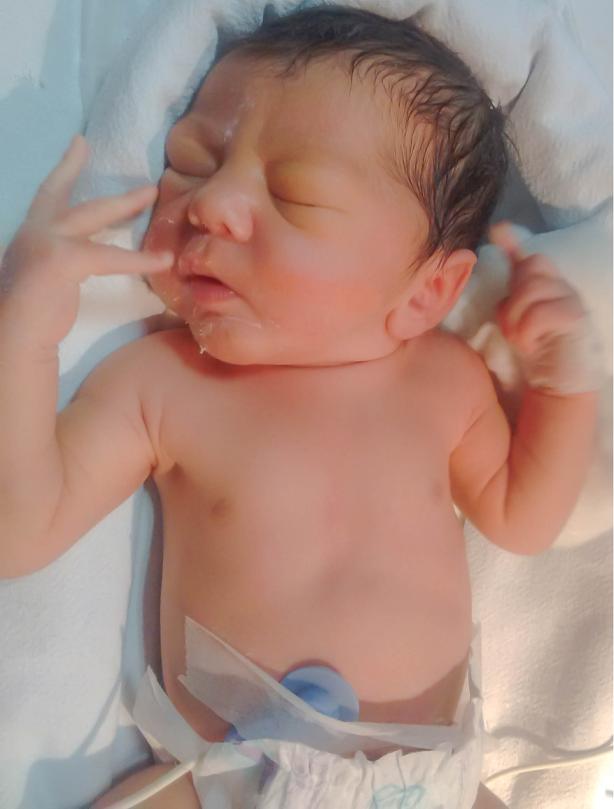
Signs:
- Hand movements of the baby increase
- Frequency of sucking actions increases
- Baby starts turning their head both ways to seek the nipple
- Baby immediately responds to anything which touches the baby's cheeks by turning the head towards it. This is called rooting
Action:
- Feed the baby in this stage without any further delay
Late Cues
If the baby stays hungry for long, the baby starts crying and becomes irritable and fussy.
Challenge:
- In this stage, the baby does not immediately accept breastfeeding
- The mother needs to hold the baby to her breasts for some time before the baby actually calms down and starts feeding
Why Crying is Not Ideal:
- Infant may be too upset to latch well
- May need calming before feeding
- Can indicate prolonged hunger
- More difficult to achieve good positioning
Calming Techniques:
- Skin-to-skin contact
- Gentle rocking or swaying
- Dimmed lighting
- Pacifying with clean finger if needed temporarily
Identifying a Sick Baby (Warning Signs)
A newborn may be ill and require immediate attention of a doctor if any of the following is present:
- Baby lethargic or unconscious
- Baby does not demand feed, or does not suckle when fed
- Baby has unusual movements (convulsions)
- Baby has fast breathing (more than 60 breaths per minute)
- Baby has chest in-drawing during breathing or makes grunting sounds while breathing
- Baby is cold on touch or has fever
- Baby's skin is blue (cyanosis) or yellow (jaundice) or less pink than usual (pale)
- Baby is not passing adequate urine (six times a day)
- Baby is excessively crying or unusually quiet
If any of the above is present, rush the newborn to a doctor immediately. The doctor will examine the baby and treat it.
Summary
Successful breastfeeding after birth requires:
-
Immediate skin-to-skin contact and early initiation of breastfeeding within the first hour
-
Appropriate positioning and attachment techniques adapted to individual needs
- Understand various positions: cradle, cross-cradle, football, side-lying
- Ensure proper latching with four key signs of good attachment
- Special consideration for cesarean section mothers
-
Recognition of feeding cues and responsive feeding practices
- Identify early cues (best time to feed)
- Respond to mid cues without delay
- Learn calming techniques for late cues
-
Assessment of feeding effectiveness using multiple indicators
- Observe during and after feeding
- Monitor daily wet diapers and stools
- Track weight gain and growth patterns
-
Safe alternative feeding methods when medically necessary
- Spoon feeding with suthi/paladai
- Cup feeding technique
- Both methods protect breastfeeding
-
Distinction between normal variations and concerning signs requiring intervention
- Know when to seek medical help
- Recognize warning signs promptly
References
-
World Health Organization. Protecting, Promoting and Supporting Breastfeeding in Facilities Providing Maternity and Newborn Services: The Revised Baby-Friendly Hospital Initiative. Geneva: WHO; 2018. Available from: https://www.who.int/publications/i/item/9789241513807
-
Moore ER, Bergman N, Anderson GC, Medley N. Early skin-to-skin contact for mothers and their healthy newborn infants. Cochrane Database Syst Rev. 2016 Nov 25;11(11):CD003519. doi: 10.1002/14651858.CD003519.pub4. Update in: Cochrane Database Syst Rev. 2025 Oct 22;10:CD003519. doi: 10.1002/14651858.CD003519.pub5. PMID: 27885658; PMCID: PMC6464366. Available from: https://pubmed.ncbi.nlm.nih.gov/27885658/
-
Widström AM, Brimdyr K, Svensson K, Cadwell K, Nissen E. Skin-to-skin contact the first hour after birth, underlying implications and clinical practice. Acta Paediatr. 2019 Jul;108(7):1192-1204. doi: 10.1111/apa.14754. Epub 2019 Mar 13. PMID: 30762247; PMCID: PMC6949952. Available from: https://pubmed.ncbi.nlm.nih.gov/30762247/
-
Flint A, New K, Davies MW. Cup feeding versus other forms of supplemental enteral feeding for newborn infants unable to fully breastfeed. Cochrane Database Syst Rev. 2016 Aug 31;2016(8):CD005092. doi: 10.1002/14651858.CD005092.pub3. PMID: 27577968; PMCID: PMC6464444. Available from: https://pubmed.ncbi.nlm.nih.gov/27577968/
-
Gartner LM, Morton J, Lawrence RA, Naylor AJ, O'Hare D, Schanler RJ, Eidelman AI; American Academy of Pediatrics Section on Breastfeeding. Breastfeeding and the use of human milk. Pediatrics. 2005 Feb;115(2):496-506. doi: 10.1542/peds.2004-2491. PMID: 15687461. Available from: https://pubmed.ncbi.nlm.nih.gov/15687461/
-
Jensen D, Wallace S, Kelsay P. LATCH: a breastfeeding charting system and documentation tool. J Obstet Gynecol Neonatal Nurs. 1994 Jan;23(1):27-32. doi: 10.1111/j.1552-6909.1994.tb01847.x. PMID: 8176525. Available from: https://pubmed.ncbi.nlm.nih.gov/8176525/
-
National Neonatology Forum India. Evidence Based Clinical Practice Guidelines. NNF India; 2022. Available from: https://www.nnfi.org/nnf-cpg-guidelines.php
-
Lawrence RA, Lawrence RM. Breastfeeding: A Guide for the Medical Profession. 9th ed. Philadelphia: Elsevier; 2021. ISBN: 978-0-323-68013-4.