Administration of Medication
Aim
To ensure safe and right administration of drugs, and to minimize medication errors.
Responsibility
Nursing Staff
SIX RIGHTS FOR ADMINISTRATION OF MEDICATIONS:
- Right patient
- Right drug
- Right dose
- Right time
- Right route
- Right documentation
BEFORE ADMINISTRATION OF MEDICATION
- Hand wash
- Check for the treatment charting prepared by the doctor. Treatment chart should be clearly legible, unambiguous, signed and dated and complete. It must specify the drug, dose, frequency, administration route and duration of administration.
- Check the medications by the name, components, dose, and expiry date.
- Check the therapeutic use, normal dosage, route of administration, potential side effects and contra-indications.
- Immediately confirm with doctor in case of any doubt in name of medicine, dose, route of administration etc.
- Confirm identification of the baby either by asking the name and age from attendants, or by checking patient identification tag.
- If necessary, assess vital parameters before and after administration of the drug.
- Document the administered medication in baby's chart.
ROUTE OF ADMINISTRATION OF MEDICATIONS
Administration of Intravenous Medications
In neonates, the administration of intravenous medications are by
- Syringe infusion pump (preferred)
- Measured Volume set (M.V. set)
- Push injections
- In neonates, medication should preferably be given via infusion pump
- Infusion pump allows slow infusion, avoiding risk of intracranial hemorrhage in neonates
Start with
- Strictly adhere to standard precautions and aseptic technique during all aspects of preparation and administration of the medication, including appropriate hand hygiene.
- Prepare the drug for administration.
- Always make sure that the drug is diluted with the right type and volume of diluents.
- Ensure that preparation of the drug is done just before the administration, otherwise the potency of medication is decreased.
- Only the nurse that prepares the medication shall administer the medication.
- Inspect I.V. site properly for sign of phlebitis.
- Administer one drug at a time and do not mix drugs together in the same infusion unless specifically prescribed, and compatibility has been confirmed by the doctor. Flush with 0.5-1.5 ml NS before, between each and after infusion to prevent incompatibility and to prevent clot formation.
- Intravenous drugs are never administered with blood or blood products.
- Administer push medications slowly, if in doubt of the rate ask the doctor.
- Observe IV cannula site frequently to minimize IV complications. Complications can cause rapid and severe tissue necrosis; it can lead to significant morbidity, functional impairment and cosmetic defects.
- Check for any reactions after the administration of drugs.
- Normal saline lock should be used after medication is given, to prevent clot formation.
All IV equipments must be changed after every 72 hours.
If possible, all parenteral drugs should be mixed under laminar air flow.
Complications
-
Infiltration: Infiltration is the inadvertent administration of a non irritant solution of medication into surrounding tissue.
Cause: IV cannula occlusion or misplacement.
Signs: Swelling and edema, pain, loss of mobility at affected limb
Prevention: Hourly monitoring of cannula site helps prevent infiltration
Treatment: Immediately remove the cannula. Apply appropriate dressing.
-
Extravasation: Extravasation is the inadvertent administration of a irritant solution of medication into surrounding tissue.
Cause: Leakage of irritant solutions into tissues, e.g., Dextrose 10%, Calcium etc.
Signs: Pain, Blistering, burning sensation, ischemia, necrosis and tissue sloughing
Prevention: Early detection and immediate action with at least hourly monitoring of the cannulation site.
Treatment: Immediately remove the cannula and apply appropriate dressing. Consult medical personnel about specific solutions and their treatment.
-
Venous spasm: Venous spasm is a sudden involuntary contraction of the vein, resulting in temporary cessation of blood flow in the vein.
Cause: Venous spasm is caused by fear and anxiety and is stimulated by cold infusates, and mechanical or chemical irritation.
Signs: Expression of pain, cramping, numbness above the infusion site
Prevention: Explain the procedure to reduce fear and anxiety. Give infusions at room temperature
Treatment: Gently massage or warm the limb and retry. Reduce the rate of infusion flow.
-
Phlebitis: Phlebitis is an acute inflammation of the intima of a vein.
Cause: Mechanical phlebitis: Large cannula, fast rate of infusion, excessive bending of arm or manipulation of cannula
Chemical phlebitis: Medications or solutions (acid or alkaline)
Bacterial / Septic phlebitis: Introduction of infectious agent at cannula site.
Signs: Expression of pain. Loss of mobility, redness, inflammation or purulent ooze at the cannula site.
Prevention: Early detection is crucial, with hourly monitoring of cannulation site.
Treatment: Stop the infusion and remove the cannula. Clean and apply a dressing. Document the incidence and treatment given.
-
Thrombophlebitis: Thrombophlebitis is the inflammation of a vein with a thrombus formation
Cause: Traumatic cannulation by an unskilled practitioner or multiple attempts. Use of too large cannula. Infusion of a high pH solution.
Signs: Local redness, hard and torturous feel of the vein, heat, painful to touch or move.
Prevention: early detection is crucial with hourly monitoring of the cannulation site. Appropriate site selection for cannulation. Appropriate cannula size selection. Skilled technique.
Treatment: Discontinue infusion, remove cannula and elevate the extremity. Document the complication and treatment given.
-
Hematoma: Hematoma is the formation of painful and hard swelling at the site of the cannula.
Cause: Infiltration of fluid in tissue at site of cannula. Excessive probing to find the vein.
Signs: Pain, swelling.
Prevention: Selection of appropriate size cannula. Skilled technique.
Treatment: Remove the cannula and apply pressure. Elevate the limb and apply a cool compress. Apply a pressure dressing if bleeding is persistent. Document the occurence of this complication.
-
Speedshock: Speedshock is a systemic reaction that occurs when a foreign substance is rapidly introduced to the circulation.
Cause: Administration of a bolus medication at a rapid rate. Can occur even if a small volume of medication is given.
Signs: Dizziness, facial flushing, headache, tightness in chest, hypotension, irregular pulse, anaphylactic shock.
Prevention: Medications must be delivered at the manufacturers recommended rate.
Treatment: The administration of medicine / infusion should be performed over the specified time. Immediately discontinue the infusion on recognition of the first symptom of speedshock and maintain the IV device for emergency intervention.
Administration of Intramuscular Injections
- Intramuscular injections are always given in the lateral aspect of the thigh in newborns.
- Do not use the gluteal region for intramuscular injections in newborns because the risk of accidental injury to sciatic nerve, resulting in paralysis of limb, is high. Moreover, gluteal muscles are under developed leading to poor absorption of medication in newborns. Never administer more than 1 ml. at one site in a newborn.
- Comfort the baby by oral administration of dextrose 10 % or sucrose 25% for pain relief before and after procedure.
PROCEDURE
- Perform hand hygiene
- Administration of Dextrose 10 % on a cotton swab two minutes prior before procedure.
- Attach a needle and load the syringe with the required and accurate dose.
- Support the baby.
- Expose the thigh and identify the injection site, lateral site of the thigh.
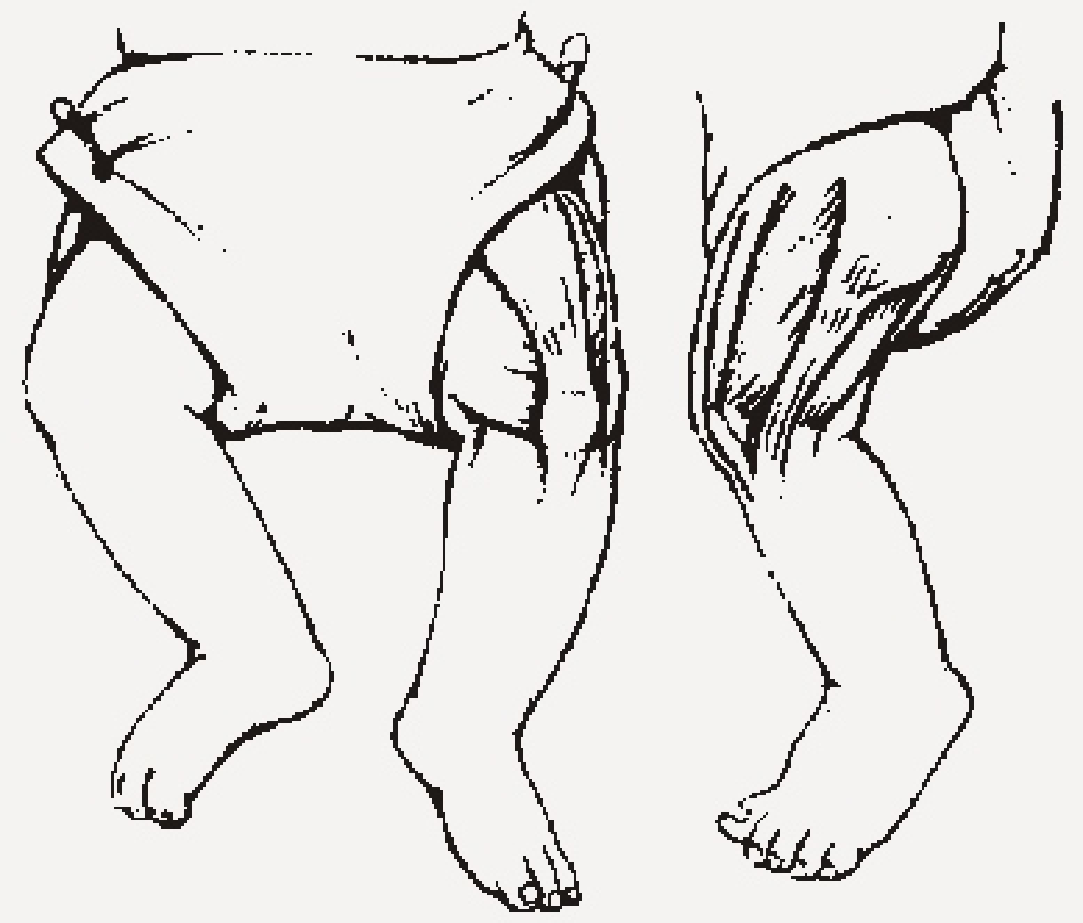
- Cleanse the site with alcohol 70 % and let it dry.
- Grasp the muscle in between thumb and the finger and insert the needle into the muscle at a right angle.
- Aspirate the syringe to see that needle is not in the blood vessel.
- Inject the required amount and withdraw the needle.
- Wipe with alcohol swab and press with dry cotton. Do not rub.
- Discard the needle in a safe container.
Administration of Subcutaneous Medications
Certain drugs are available in heavy suspensions and can be safely injected in small amount subcutaneously.
The sites are same as we use in IM injections, additional areas of loose areolar tissue can be used.
For the subcutaneous administration, a small or tuberculin syringe is used and inserted in 45 degree angle holding the pinch of skin firmly between the thumb and index finger. The advantage of subcutaneous route include the presence of many sites for injection and rotation and there is less chance of damage of nerves and blood vessels. Remember to wipe the skin with alcohol 70 % prior to puncturing, and support and give pain relief with 10 % dextrose to the baby during the procedure.
DISPLACEMENT VALUES FOR IV ANTIBIOTICS
| DRUG | DISPLACEMENT VOLUME | VOLUME OF DILUENT TO BE ADDED | FINAL VOLUME | FINAL CONCENTRATION |
|---|---|---|---|---|
| Aciclovir 250 mg | Negligible | 10 mL | 10 mL | 25 mg/mL |
| Amoxicillin-clavulanate 625 mg | 0.5 mL | 9.5 mL | 10 mL | 62.5 mg/mL |
| Aztreonam 1 g | 1.1 mL | 3.9 mL | 5 mL | 200 mg/mL |
| Cefotaxime 1 g | 0.5 mL | 4 mL | 4.5 mL | 220 mg/mL |
| Ceftazidime 1 g | 0.9 mL | 9.1 mL | 10 mL | 100 mg/mL |
| Ceftriaxone 1 g | 0.5 mL | 9.5 mL | 10 mL | 100 mg/ mL |
| Cefuroxime 750 mg | 0.5 mL | 7 mL | 7.5 mL | 100 mg/mL |
| Meropenem 500 mg 1 g | 0.4 mL 0.9 mL | 9.6 mL 19.1 mL | 10 mL 20 mL | 50 mg/mL 50 mg/mL |
| Piperacillin / Tazobactam 2.25 g | 1.5 mL | 8.5 mL | 10 mL | 225 mg/mL |
| Vancomycin 500 mg | 0.32 mL | 9.68 mL | 10 mL | 50 mg/mL |
VISUAL PHLEBITIS SCORE
| Condition of Site | Score | Degree of Phlebitis |
|---|---|---|
| IV Site appears healthy | 0 | No signs of phlebitis |
| One of the following is evident: Slight discomfort at IV site Slight swelling at IV site | 1 | First signs of phlebitis Observe cannula |
| Two of the following are evident: Pain at IV site Erythema Swelling | 2 | Early stages of phlebitis Resite cannula |
| All of the following are present: Pain along path of cannula Erythema Induration | 3 | Medium stages of phlebitis Resite cannula Consider treatment |
| All of the following sites are evident: Pain along path of cannula Erythema Induration Palpable venous cord | 4 | Advanced stages of phlebitis, or the start of Thrombophlebitis Resite cannula Consider treatment |
| All of the following sites are evident: Pain along path of cannula Erythema Induration Palpable venous cord Pyrexia | 5 | Advanced stages of Thrombophlebitis Initiate treatment Resite cannula |
References
- Core Curriculum for Neonatal Intensive Nursing by Verklan & Walden, 3rd edition (2004)
Practical Procedures for the Newborn Nursery - Deorari, Paul, Singhal et.al, 3rd edition (2010)
Pediatric Nursing by Datta, 2nd edition (2009) - Neonatal Intensive Care by Merenstein and Gardner, 7th edition (2011)
- Comprehensive Neonatal Nursing Care by Kenner and Lott, 5th edition (2014)
- Jackson, A. A battle in vein-infusion phlebitis. Nursing Times 1998; 94(4)in SARI Prevention Of Intravascular Catheter related Infection Sub-Committee.
Document Information
Version: 2.0
Published: August 20, 2015
Revised by: Dr Chetan Meena
Contributors: Nurse Ajeeta George, JK Lone Hospital, SMS Medical College, Jaipur
Previous Versions: v1.0